The value of vaccines in Ireland

Vaccination is one of the most cost-effective health interventions available, saving millions of people from illness, disability and death each year. The World Health Organization (WHO) states a comprehensive vaccination programme is a cornerstone of good public health in any country.
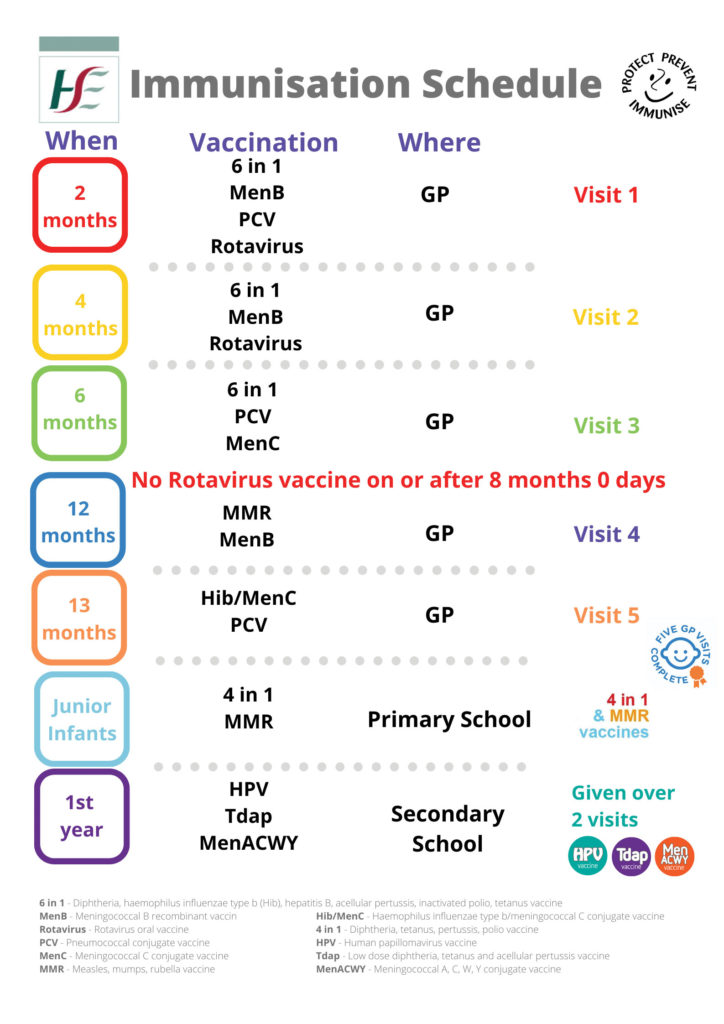
In Ireland today, vaccines are offered to children to protect against 13 diseases: diphtheria, haemophilus influenzae
type b (Hib), hepatitis B, HPV infection, measles, meningococcal disease (types A, B, C, W & Y), mumps, pertussis (whooping cough), pneumococcal, polio, rotavirus, rubella and tetanus. These diseases may result in serious complications including death. Outbreaks of these serious infectious diseases occur if children are not vaccinated.

Vaccines have an excellent safety record. All medicines can cause side effects, vaccine side effects are usually mild, like a sore arm or leg where the injection was given, or a slight fever. Serious side effects to vaccines are extremely rare. All of the recommended vaccines used in Ireland are licensed by the Health Products Regulatory Authority (HPRA) or the European Medicines Agency. They are licensed for use only when they have been shown to be both safe and effective.
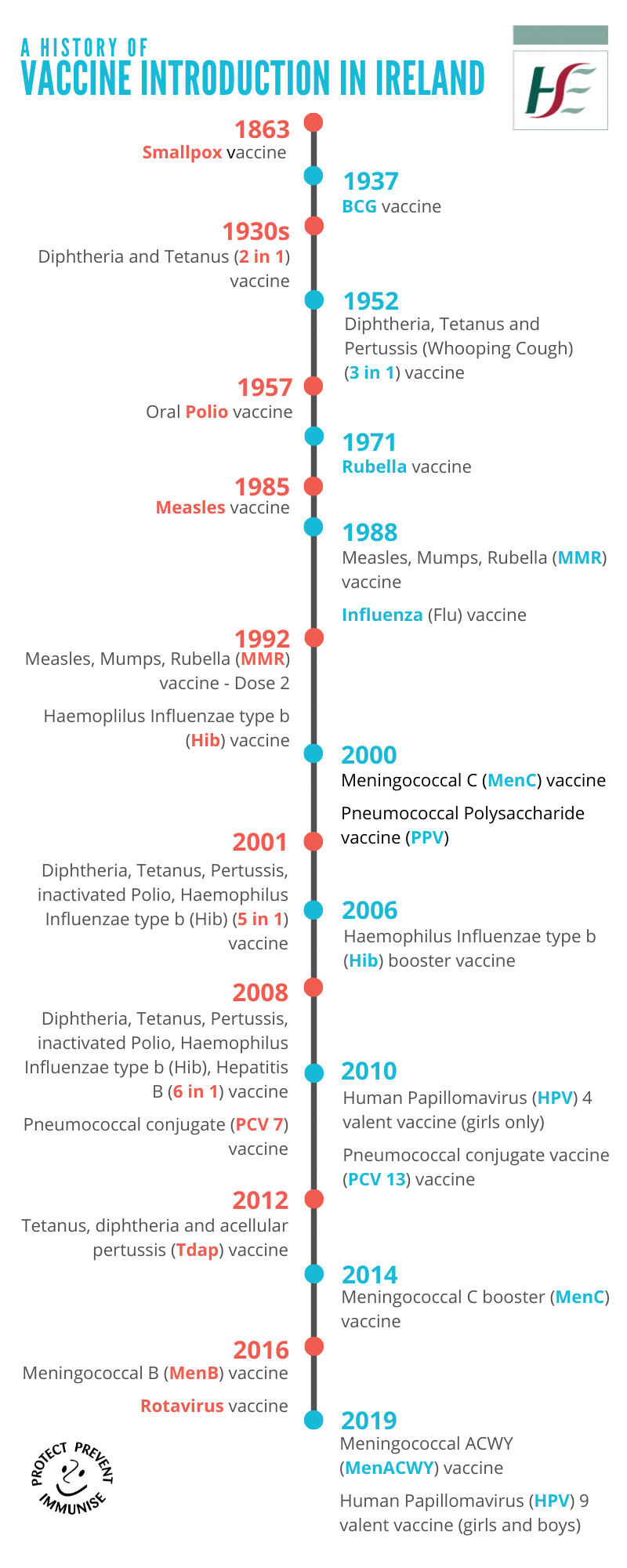
Though vaccination is often presented as a very modern development, there have been government funded Public Health vaccination programmes in Ireland for 180 years.
1800s
In 1863 vaccination against smallpox was made compulsory for all children born in Ireland. Parents were given responsibility to ensure vaccination of infants against smallpox within six months of birth.
Deaths caused by smallpox began to fall, from 7,550 for the decade from 1871 to 1880 until the last reported death from smallpox in Ireland was reported in 1907. Smallpox vaccination stopped in Ireland in 1972. WHO declared smallpox eradicated worldwide in 1979.
1930-1940s
Diphtheria, ‘the strangling angel of children’, was a terrifying disease that suffocated a child. Diphtheria was a very common cause of death among children until the 1940s in Ireland.
In 1938, there were several thousand cases of diphtheria with 318 deaths reported. With the introduction of diphtheria and tetanus vaccine, the number of deaths fell year on year during the 1940s. In 1950 there were five deaths from diphtheria. The last death notified from diphtheria in Ireland was in 1967. Deaths still occur in unvaccinated children in Western Europe.
1950s
Pertussis (Whooping cough) vaccine was added to the diphtheria/tetanus vaccines and offered to all children from 1953.
Prior to the introduction of a whooping cough vaccine there were up to 5,000 cases of pertussis and up to 200 deaths each year from whooping cough. Following the introduction of the vaccine, cases and deaths from whooping cough fell rapidly.
Today, due to an increase in whooping cough cases, pregnant women are recommended to receive the vaccine between 16 and 36 weeks of pregnancy to protect their baby from this serious disease when they are too young to be fully vaccinated.
Polio has existed for thousands of years and epidemics were first reported in the 1800s. Polio maimed, rather than killed and mainly affected children under 3 years of age causing long term paralysis. In Ireland, polio infection became more common after 1920 with major polio epidemics during the 1940s and 1950s. The last and most severe polio epidemic took place in 1956 when there were 500 cases reported, mostly children, with 220 cases from Cork.
In 1955, Dr Jonas Salk produced a vaccine for poliomyelitis. The Salk vaccine was introduced in Ireland in 1957. A few years after introduction of universal childhood vaccination, polio infection was almost eliminated. The last reported case of polio here was in 1984. However, over 7,000 people still suffer from post-polio syndrome in Ireland and cases of polio still occur in other parts of the world.
1970s
During the 1950s and 1960s up to 5,000 cases of rubella were reported during epidemics. Rubella vaccine was introduced here in 1971. Rubella infection in early pregnancy has serious effects on the foetus causing cataracts, congenital heart disease, hearing impairment and developmental delay. Prevention of these abnormalities (congenital rubella syndrome) is main aim of rubella vaccination. In 2016, a WHO declaration stated that following vaccination rubella is no longer endemic in Ireland.
1980s
Before 1984, an average of 5,000 cases of measles were reported annually in Ireland. In 1948 there were 63 deaths from measles and due to advances in hospital care by 1985 there were 5 deaths reported. The number of cases of measles declined dramatically after introduction of measles vaccine in 1985, from 10,000 cases in 1985 to 201 cases in 1987. MMR (measles, mumps and rubella) vaccine was introduced to Irish childhood immunisation schedule in 1988. However, measles outbreaks still occur in Ireland. The largest in recent years occurred in 2000, when more than 1,600 cases were reported and three children died.
1990s to present day
In 1999, there were 536 cases of meningitis caused by meningococcal infection and two cases of meningitis caused by haemophilus influenzae type b reported. More than 100 cases of meningitis caused by haemophilus influenzae type b were reported most years before introduction of haemophilus influenzae type b (Hib) vaccine in 1992. The meningococcal C vaccine was introduced in 2000, and meningococcal B vaccine was introduced in 2016. Cases of meningococcal meningitis have dropped more than 80 per cent since these vaccines were introduced.
In 2010, HPV vaccine was introduced for girls to prevent cervical cancer and in 2019 this was extended to include first year boys to protect them against cancers and genital warts caused by HPV virus.
The rotavirus vaccine was introduced in 2016 to prevent severe diarrhoea in children. Reported cases of rotavirus infection fell by more than 70 per cent in 2018.
Why do we still have outbreaks?
The World Health Organization recommends a target uptake of 95 per cent for childhood vaccines to protect the entire population. Ireland has reached the target uptake for some childhood vaccinations including diphtheria, tetanus, pertussis, polio, and hepatitis B vaccines. However, the target uptake for measles, mumps, rubella, meningococcal, Hib and rotavirus vaccinations have not been reached.
As the Covid-19 pandemic has shown, infectious diseases are only a plane ride away. So if a visitor to Ireland has a measles infection, an outbreak of measles can easily occur because 95 per cent of all children are not vaccinated.
Almost 200 years of vaccination campaigns delivered to millions of people have greatly reduced the burden of infectious diseases that killed and maimed children and adults in Ireland, however it is important to remember that other than smallpox these diseases have not gone away yet.
Vaccination provides the best protection against these serious diseases.
More Information
W: www.immunisation.ie
Twitter: @hseimm






