Medicine management

Following a move by the Health Minister to unilaterally cut the price the HSE pays for drugs earlier this year, eolas examines the fundamentals of the Health (Pricing and Supply of Medical Goods) Act 2013 and changes it has helped introduce.
As Ireland’s population continues to increase, so too does the living age of the population, placing additional pressure on the health service. Consequently, reducing Government’s expenditure on the spiralling cost of drugs in Ireland has presented a major challenge for Health Minister Simon Harris.
In 2015 alone it was estimated that Government allocated around €1.7 billion from the health budget on drugs and it is believed that prices are set to rise by €100 million annually. The HSE is committed to saving over €110 million on drugs annually but earlier this year talks between the State and pharmaceutical companies to compromise on price reductions broke down. It is expected that the enforced drop will force further talks for an agreed deal on lower prices.
The issue of expensive drugs was raised again earlier this year over the drug Orkambi, a treatment that helps improve the lives of people living with Cystic Fibrosis. The Government has been criticised for not yet signing off on the drug after the National Centre for Pharmacoeconomics declared the €160,000 per patient cost too expensive.
The ability of the HSE to set reimbursement prices was established by the Health (Pricing and Supply of Medical Goods) Act 2013, a move by the previous government to reduce drug costs under the ‘Future Health’ reform 2012-2015.
The need for a change in the way medicines were dispensed and reimbursed in Ireland were highlighted by the 2010 figure that Ireland was the third highest spender of 25 EU countries in pharmaceuticals per capita.
The 2013 Act introduced changes as to how medicine would be dispensed and the way in which prices are set in Ireland. Simultaneously, it established the HSE’s Medicines Management Programme in 2013 to optimise prescribing through evidence and cost, while prioritising patient safety.
The Act defined a reimbursement list by the HSE, outlining provision procedures for reimbursable medicines under the community drug schemes. Entry on to the list required clinical and cost-effectiveness evidence and the Act set out that the HSE was responsible for agreeing the price of medicines on the list with pharmaceutical companies. The list also included items that were ‘interchangeable’, whereby the HSE could agree a reference price, even if a medication is substituted.
These interchangeable medicines can also be described as generic medicines, having “the same qualitive and quantitative composition in active substances(s) as a medicine that has already been authorised”.
The list of interchangeable medicines is published on the Health Products Regulatory Authority (HPRA) website and the value of the Act lies in allowing pharmacists to substitute a less expensive medicine from within the list. It also allows for the HSE to set a reference price for interchangeable medicines, meaning that only the reference price will be reimbursed no matter what medicine within the group is dispensed.
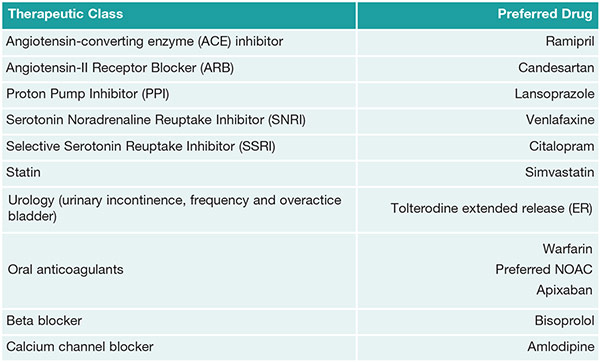
Medicines Management Programme (MMP)
Set up as part of the 2013 Act to encourage evidence-based prescribing the MMP is supported by experts from several national bodies. The most significant arm of the Programme lies in the preferred drugs initiative, which offers prescribers guidance on the best drug for a particular condition. An extensive review of every drug is conducted before the preferred drug is identified and then made available to prescribers. The aim of the programme is to increase awareness among prescribers and healthcare professionals around cost and encourage use of less expensive, but “equally effective” therapies for patients where possible.